Monkeypox frequently asked questions: Cause, symptoms, transmission, treatment and all you need to know
New Delhi, May 21: The World Health Organization (WHO) has announced that a total of 80 cases of monkeypox in 11 countries have been reported and said they are working to better understand the extent and cause of the outbreak.
Recommended Video
In a statement issued on Friday, the WHO said the virus is endemic in some animal populations in a number of countries, leading to occasional outbreaks among local people and travelers. "WHO and partners are working to better understand the extent and cause of an outbreak of monkeypox. The virus is endemic in some animal populations in a number of countries, leading to occasional outbreaks among local people and travellers.
The WHO has also released a list of frequently asked questions and answers.
What is Monkeypox?
Monkeypox is a disease caused by the monkeypox virus. It is a viral zoonotic disease, meaning that it can spread from animals to humans. It can also spread between people.
Where is Monkeypox typically found?
Monkeypox is commonly found in Central and West Africa where there are tropical rainforests and where animals that may carry the virus typically live. People with monkeypox are occasionally identified in other countries outside of Central and West Africa, following travel from regions where monkeypox is endemic.
Where are the symptoms of Monkeypox?
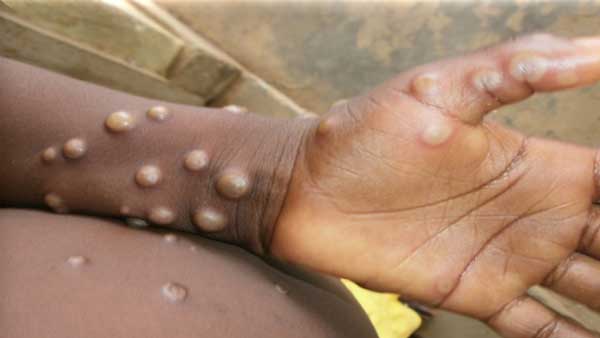
Symptoms of monkeypox typically include a fever, intense headache, muscle aches, back pain, low energy, swollen lymph nodes and a skin rash or lesions. The rash usually begins within one to three days of the start of a fever. Lesions can be flat or slightly raised, filled with clear or yellowish fluid, and can then crust, dry up and fall off. The number of lesions on one person can range from a few to several thousand. The rash tends to be concentrated on the face, palms of the hands and soles of the feet. They can also be found on the mouth, genitals, and eyes.
Symptoms typically last between two to four weeks and go away on their own without treatment. If you think you have symptoms that could be monkeypox, seek advice from your health care provider. Let them know if you have had close contact with someone who has suspected or confirmed monkeypox.
Can people die from Monkeypox?
In most cases, the symptoms of monkeypox go away on their own within a few weeks, but in some individuals, they can lead to medical complications and even death. Newborns, children and people with underlying immune deficiencies may be at risk of more serious symptoms and death from monkeypox.
Complications from severe cases of monkeypox include skin infections, pneumonia, confusion, and eye infections which can lead to loss of vision. Around 3 - 6% of reported cases have led to death in endemic countries in recent times, often in children or persons who may have other health conditions. It is important to note that this may be an overestimate because surveillance in endemic countries is limited.
How does monkeypox spread from animals to humans?
Monkeypox can spread to people when they come into physical contact with an infected animal. Animal hosts include rodents and primates. The risk of catching monkeypox from animals can be reduced by avoiding unprotected contact with wild animals, especially those that are sick or dead (including their meat and blood). In endemic countries where animals carry monkeypox, any foods containing animal meat or parts should be cooked thoroughly before eating.
How does monkeypox spread from person to person?
People with monkeypox are infectious while they have symptoms (normally for between two and four weeks). You can catch monkeypox through close physical contact with someone who has symptoms. The rash, bodily fluids (such as fluid, pus or blood from skin lesions) and scabs are particularly infectious. Clothing, bedding, towels or objects like eating utensils/dishes that have been contaminated with the virus from contact with an infected person can also infect others.
Ulcers, lesions or sores in the mouth can also be infectious, meaning the virus can spread through saliva. People who closely interact with someone who is infectious, including health workers, household members and sexual partners are therefore at greater risk for infection.
The virus can also spread from someone who is pregnant to the foetus from the placenta, or from an infected parent to child during or after birth through skin-to-skin contact.
It is not clear whether people who do not have symptoms can spread the disease.
Who is at risk of catching monkeypox?
Anyone who has close physical contact with someone who has symptoms of monkeypox, or with an infected animal are at highest risk of infection. People who were vaccinated against smallpox are likely to have some protection against monkeypox infection. However, younger people are unlikely to have been vaccinated against smallpox because smallpox vaccination stopped worldwide after smallpox became the first human disease to be eradicated in 1980. Even though people who have been vaccinated against smallpox will have some protection against monkeypox, they also need to take precautions to protect themselves and others.
Newborns, children and people with underlying immune deficiencies may be at risk of more serious symptoms and death from monkeypox. Health workers are also at higher risk due to longer virus exposure.
How can I protect myself and others against monkeypox?
You can reduce your risk by limiting contact with people who have suspected or confirmed monkeypox.
If you do need to have physical contact with someone who has monkeypox because you are a health worker or live together, encourage the infected person to self-isolate and cover any skin lesion if they can (e.g., by wearing clothing over the rash). When you are physically close to them, they should wear a medical mask, especially if they are coughing or have lesions in their mouth. You should wear one also. Avoid skin-to-skin contact whenever possible and use disposable gloves if you have any direct contact with lesions. Wear a mask when handling any clothes or bedding if the person cannot do it themselves.
Regularly clean your hands with soap and water or an alcohol-based hand rub, especially after contact with the person who is infected, their clothes, bed sheets, towels and other items or surfaces they have touched or that might have come into contact with their rash or respiratory secretions (e.g., utensils, dishes). Wash the person's clothes, towels and bedsheets and eating utensils with warm water and detergent. Clean and disinfect any contaminated surfaces and dispose of contaminated waste (e.g., dressings) appropriately.
Can children get monkeypox?
Children are typically more prone to have severe symptoms than adolescents and adults. The virus can also be passed to a foetus or to a new born through birth or early physical contact.
What should I do if I think I may have monkeybox?
If you think you have symptoms or have been a close contact of someone with monkeypox, contact your health worker for advice, testing and medical care. If possible, self-isolate and avoid close contact with others. Clean hands regularly and take the steps listed above to protect others from infection. Your health worker will collect a sample from you for testing so that you can get appropriate care.
Is there a vaccine against monkeybox?
There are several vaccines available for prevention of smallpox that also provide some protection against monkeypox. A newer vaccine that was developed for smallpox (MVA-BN - also known as Imvamune, Imvanex or Jynneos) was approved in 2019 for use in preventing monkeypox and is not yet widely available. WHO is working with the manufacturer to improve access. People who have been vaccinated against smallpox in the past will also have some protection against monkeypox. The original smallpox vaccines are no longer available to the general public, and people below the age of 40 - 50 years are unlikely to have been vaccinated, since vaccination against smallpox ended in 1980 after it became the first disease to be eradicated. Some laboratory personnel or health workers may have been vaccinated with a more recent smallpox vaccine.
Is there a treatment for monkeypox?
Monkeypox symptoms often resolve on their own without the need for treatment. It is important to take care of the rash by letting it dry if possible or covering with a moist dressing to protect the area if needed. Avoid touching any sores in the mouth or eyes. Mouth rinses and eye drops can be used as long as cortisone-containing products are avoided. Vaccinia immune globulin (VIG) may be recommended for severe cases. An antiviral that was developed to treat smallpox (tecovirimat, commercialized as TPOXX) was also approved for the treatment of monkeypox in January 2022.
Where in the world is there currently a risk of monkeypox?
Since 1970, human cases of monkeypox have been reported in 11 African countries - Benin, Cameroon, the Central African Republic, the Democratic Republic of the Congo, Gabon, Côte d'Ivoire, Liberia, Nigeria, the Republic of the Congo, Sierra Leone, and South Sudan.
Cases occur occasionally in non-endemic countries. These are typically reported in persons who have travelled to endemic countries. One outbreak was caused by contact with animals who had been infected by other imported small mammals.
In May 2022, multiple cases of monkeypox are being identified in several non-endemic countries. This is not typical of past patterns of monkeypox. WHO is working with all affected countries to enhance surveillance and provide guidance on how to stop the spread and how to care for those infected.
What do we know about the outbreak of monkeypox identified in several countries in May 2022?
Several countries where monkeypox is not endemic have reported cases in May 2022. As of 19 May 2022, cases are being reported from over 10 countries in non-endemic areas. Additional cases are being investigated. For the latest information, please see here.
With the exception of cases sporadically reported in travellers from endemic countries, cases in non- endemic areas that are not linked to travel from endemic countries are not typical. At the present time (as of May 2022) there is no clear link between the cases reported and travel from endemic countries and no link with infected animals.
We understand that this outbreak is concerning for many, especially people whose loved ones have been affected. What is most important right now is that we raise awareness about monkeypox among people who are most at risk of infection and provide advice on how to limit further spread between people. It is also important that public health workers are able to identify and care for patients. It is essential that no one stigmatize anyone who is affected by this event. WHO is working to support Member States with surveillance, preparedness and outbreak response activities for monkeypox in affected countries.
Studies are underway in affected countries to determine the source of infection of each identified case, and actions to provide medical care and limit further spread.
Is there a risk of this becoming a larger outbreak?
Monkeypox is not typically considered to be very contagious because it requires close physical contact with someone who is infectious (e.g., skin to skin) to spread between people. The risk to the general public is low. WHO is responding to this outbreak as a high priority to avoid further spread; for many years has considered monkeypox a priority pathogen. The cases we are currently seeing are not typical for outbreaks of monkeypox because there is no reported travel from endemic countries or to animals exported from endemic countries. Identifying how the virus is spreading and protecting more people from becoming infected is a priority for WHO. Raising awareness about this new situation will help to stop further transmission.
Is monkeypox a sexually transmitted disease?
Monkeypox can spread from one person to another through close physical contact, including sexual contact. It is currently not known whether monkeypox can be spread through sexual transmission routes (e.g., through semen or vaginal fluids), but direct skin-to-skin contact with lesions during sexual activities can spread the virus.
Monkeypox rashes are sometimes found on genitals and in the mouth, which is likely to contribute to transmission during sexual contact. Mouth-to-skin contact could thus cause transmission where skin or mouth lesions are present.
Monkeypox rashes can resemble some sexually transmitted diseases, including herpes and syphilis. This may explain why several of the cases in the current outbreak have been identified amongst men seeking care in sexual health clinics.
The risk of becoming infected with monkeypox is not limited to people who are sexually active or men who have sex with men. Anyone who has close physical contact with someone who is infectious is at risk. Anyone who has symptoms that could be monkeypox should seek advice from a health worker immediately.
Are men who have sex with men at higher risk of catching monkeypox?
Monkeypox is spread from person to person through close physical contact. The risk of monkeypox is not limited to people who are sexually active or men who have sex with men. Anyone who has close physical contact with someone who is infectious is at risk. Anyone who has symptoms that could be monkeypox should seek advice from a health care provider immediately. This includes people who have connections to communities where cases have been reported.
Several of the cases that have been reported from non-endemic countries have been identified in men who have sex with men. These cases were identified at sexual health clinics. The reason we are currently hearing more reports of cases of monkeypox in communities of men who have sex with men may be because of positive health seeking behaviour in this demographic. Monkeypox rashes can resemble some sexually transmitted diseases, including herpes and syphilis, which may explain why these cases are being picked up at sexual health clinics. It is likely that as we learn more, we may identify cases in the broader community.
What is WHO's response to stigmatising messaging circulating online related to monkeypox?
We have seen messages stigmatising certain groups of people around this outbreak of monkeypox. We want to make it very clear that this is not right. First of all, anyone who has close physical contact of any kind with someone who has monkeypox is at risk, regardless of who they are, what they do, who they choose to have sex with or any other factor. Secondly, stigmatising people because of an illness or a disease is unacceptable. Stigma is only likely to make things worse and stop us from ending this outbreak as fast as we can. We need to all pull together to support anyone who has been infected or who is helping to take care of people who are unwell. We know how to stop this disease, and how we can all protect ourselves and others. Stigma and discrimination is never ok, and it is not ok in relation to this outbreak. We are all in this together.
Why is this disease called monkeypox?
The disease is called monkeypox because it was first identified in colonies of monkeys kept for research in 1958. It was only later detected in humans in 1970.
Source: WHO















 Click it and Unblock the Notifications
Click it and Unblock the Notifications